This is What Not Giving Up Looks Like

“My family said he was too tiny – he would die with surgery and die without surgery. They told me not to bother taking Djaliou to the ship,” recounted Sara…
Remembering when she was first told her son could have a free operation onboard the Africa Mercy. The five-month-old was born with a rare condition, something most of our surgeons had only read about. A mass on the infant’s tongue, present since birth, made it difficult for him to breathe or eat – which made it nearly impossible for him to grow. The energy the baby got from his mother’s milk was mostly used just to get air into his body. Whenever he inhaled, his ribcage would shudder as if he were taking his last breath.
But even with the odds against her little boy, Sara persisted. Although he couldn’t breastfeed, she was able to manually pump milk for him – but even then, Djaliou drank little. And, although most of her family advised Sara to give up her son as dead, her husband thought differently. “Go to the ship,” he said. So Sara packed a few things and made the ten-hour trek, with her silent baby – he had no strength to cry – tucked close.

But upon coming to the ship, Djaliou wasn’t a “quick fix.” His relatives had been right – at 4.7 pounds, the 3-month-old weighed far too little for surgery. Even though it was difficult for him to eat, he had to gain weight for any chance to live. For almost two months, Djaliou and his mother stayed at the HOPE Center, the Mercy Ships outpatient facility, working regularly with Lee-Anne Borrow (AUS), a volunteer dietician and the head of the Africa Mercy Infant Feeding Program. Slowly, the baby put on weight.
Even so, Sara remained ambivalent. “I always had two ideas in my head,” she recounted. “Sometimes I thought my baby would die. Sometimes I thought he would live …”
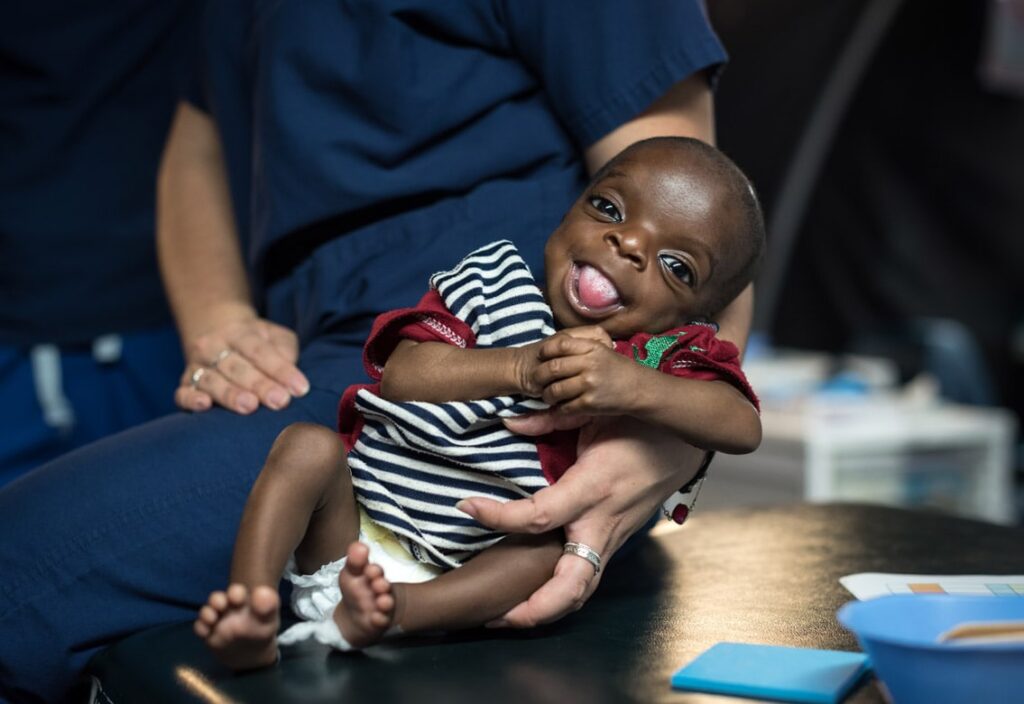
And perhaps Sara was right to remain cautious – even though Djaliou was closer and closer to being ready for surgery, such a specialized operation would require just the right group of experts, experts who were not yet onboard the Africa Mercy.
But then, almost two months after Sara had brought her son to the ship, the perfect scenario developed. “It’s really incredible,” said Lee-Anne. “We had an Ear Nose and Throat specialist and a Pediatric Anesthesiologist overlap here for a short window of time – they were exactly who we needed.”
Within a few days, Djaliou was whisked onboard the Africa Mercy – he would have surgery the following morning. But that night, even as the ward grew silent, the voices of Sara’s family began to echo through the mother’s head. “I did not sleep,” she recounts. “I was remembering what people had said – that my son would die during the operation.”

The next day, the operating team worked from morning till night, slowly removing the mass from Djaliou’s tongue. All the while, Sara waited, speaking very little to anyone. But, as evening approached, she was finally called into the recovery room. There was her son, Djaliou – alive.
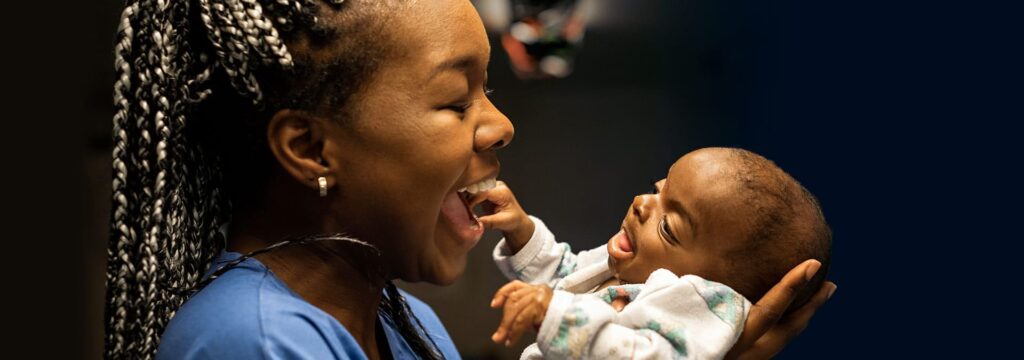
A week after surgery, Sara sat next to Lee-Anne, watching as her son played with the dietician’s Africa Mercy badge. Djaliou had recovered quickly, and it was already his second-to-last checkup. Immediately after the operation, his breathing became much easier, and he began crying like a normal baby. Within a few days, he was even able to drink by himself.
“Now I’m just waiting until you’ll tell me I can go home,” Sara said with a laugh, looking at her son as he cooed. “I want to show everyone he is alive.”

The Woman Who Forged Her Way Through Walls: Florence Bangura’s Story
Florence’s journey from oldest to newest Mercy Ship came full circle when she met the Global Mercy™ in 2023, the same year that the purpose-built hospital ship began welcoming its patients on board. Today, you can find Florence, now 49 years old, down in the engine room as a hotel engineering assistant.

Transforming Sierra Leone’s Healthcare: A Vision for Safe and Affordable Surgery
As experts from the surgical and healthcare world gather for the 64th Annual Conference and Scientific Meeting of the West African College of Surgeons in Sierra Leone this week, a profound dedication to advancing surgical knowledge and practice in the region is palpable. At the forefront of discussions lies the conference’s pivotal theme: access to safe and affordable surgical and anesthetic care in West Africa. This theme highlights the pressing need to address disparities in healthcare capabilities and capacities across the region, especially the critical importance of equitable access to quality surgical interventions.

The Africa Mercy Arrives in Madagascar to Bring Hope and Healing Anew
Freshly refitted hospital ship, the upgraded Africa Mercy® has arrived at the island nation to build on the charity’s longstanding collaboration and will provide specialized surgeries in various fields, including maxillofacial and ear nose and throat, general, pediatric specialized general, pediatric orthopedic, cataract surgery, and reconstructive plastics.

Reuniting with Vanya, Years After Surgery
In 2015, in an operating room on board the Africa Mercy while docked in Madagascar, the course of Vanya’s life changed.
Years have now passed since Vanya’s journey toward healing. In the time since, her improved ability to walk allowed her to return to school, where she loved studying environmental science and learning about the world around her.

Christmas-Thank You Message from Darryl Anderson
Darryl Anderson shares his thank you message after Christmas to express his gratitude for your support and dedication to our mission.

Kadidja: A Future as Bright as her Smile
At Mercy Ships Canada, we serve those who have lost hope, bringing healing and transformation. Our volunteers, inspired by their faith, work selflessly to perform surgeries that renew not only bodies but also faith and hope. This Christmas, be a part of the miracle by making a donation to Mercy Ships Canada. Your contribution will help renew faith and offer a second chance at life. Together, we can make a significant impact on those who have suffered for too long.
Share
Related Posts

A Promise Fulfilled: The Africa Mercy Returns to Africa
The Africa Mercy® hospital ship returned to West Africa, bringing hope and healing as the vessel docked once again in the port of Dakar, Senegal.

Africa Celebration
The Africa Celebration is a moment to pause and give thanks for 30 years of partnership, filled with stories of hope and healing.

International Symposium and Dakar Declaration
Learn more about the International Symposium and Dakar Declaration that were hosted in Dakar, Senegal, on Friday, May 6, 2022.

A Franco-Canadian Onboard the Global Mercy
Now living in France, Léa works for Mercy Ships Canada remotely and “seized the opportunity” when the hospital ship Global Mercy came to Europe.
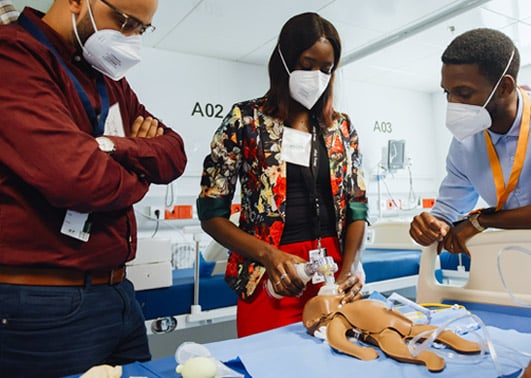
Safer Surgery for a New Generation: Pediatric Anesthesia Training in Senegal
In June 2022, more than 30 Senegalese healthcare professionals boarded the Global Mercy® to equip themselves with new skills that could save countless vulnerable young lives.

NOTICE OF BOARD VACANCIES MERCY SHIPS CANADA
Mercy Ships Canada is seeking up to three dynamic independent Directors to join our Board over the next 18-months.
